A survey study of index food-related allergic reactions and anaphylaxis management
Thanks in large part to the enthusiastic and committed members of KFA, we recently published an article in the journal Pediatric Allergy and Immunology (now available online, and soon to be in print); this article seeks to portray reactions that food-allergic children experience, as well as how these reactions are managed by physicians and other health care providers.
Food-related allergic reactions include a spectrum of presentations, with anaphylaxis being the most severe manifestation. Food allergy is the leading cause of anaphylaxis in children, and is responsible for approximately half of reported anaphylaxis cases presenting to emergency departments. The incidence of food-induced anaphylaxis has been increasing, particularly within the pediatric population. Unfortunately, initial food allergic reactions are often poorly recognized and under-treated, and in general there is limited prior study of the management of anaphylaxis in pediatric populations.
In this survey study we were interested not only in looking at symptoms children experience with food allergic reactions, but also at how well the medical community is doing at managing these reactions.
We thought that the best way to look at medical management of reactions would be to examine initial reactions that led families to seek urgent medical care for the first time, since after children are known to be food allergic and their families become educated, family members may be more likely either to provide appropriate treatment at home or to influence the way their children are managed in doctors’ offices, ambulances, emergency departments, urgent care centers, etc.
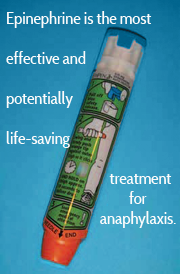
We invited parents of food-allergic children to complete an online questionnaire, designed with Kids with Food Allergies Foundation, about their children’s first food-allergic reactions resulting in urgent medical evaluation. Among 1361 initial reactions, about three quarters of the reactions were highly likely to represent anaphylaxis. Surprisingly, only one-third of these reactions were treated with intramuscular epinephrine, which is the most effective and potentially life-saving treatment for anaphylaxis, and should represent the cornerstone of treatment. As expected, when epinephrine was administered, about three quarters of the time it was done so by emergency department physicians or paramedics. About one tenth of the time epinephrine was given in primary care physicians’ offices, which emphasizes the importance of anaphylaxis education and emergency preparedness in office or clinic settings.
• Infants
• Children having reactions to milk or egg
• Children with symptoms of abdominal pain and/or diarrhea
We found that anaphylactic reactions were more likely to be missed or under-treated with epinephrine in several groups of children: infants, children experiencing reactions to milk or egg ingestions, and children with symptoms of abdominal pain and/or diarrhea. Epinephrine was more likely to be given to children with asthma, as well as to children with peanut or tree nut reactions.
Another concerning finding was that of children treated with epinephrine, only half reported being prescribed epinephrine auto-injectors; having an auto-injector available is crucial in case of symptom recurrence or repeat exposure prior to formal allergy evaluation. Furthermore, fewer than half of these patients were referred to allergists.
Previous studies have highlighted problems involving under-prescription and under-utilization of epinephrine in anaphylaxis management. Despite growing awareness of food allergy in the general and medical communities, our study suggests that these shortcomings persist. We are grateful to KFA and its members for making this study possible. Our hope is that it leads to increased awareness and opportunities for education about recognition and treatment of food-induced anaphylactic reactions.
Reference:
Jacobs, T. S., Greenhawt, M. J., Hauswirth, D., Mitchell, L. and Green, T. D. (2012), A survey study of index food-related allergic reactions and anaphylaxis management. Pediatric Allergy and Immunology. doi: 10.1111/j.1399-3038.2012.01315.x
Tammy Jacobs, M.D., is a pediatrics resident and soon-to-be fellow in allergy/immunology at Children's Hospital of Pittsburgh of University of Pittsburgh Medical Center. Todd Green, M.D., F.A.A.P, F.A.A.A.A.I., is a member of the KFA Medical Advisory Team, as well as an allergist/immunologist and assistant professor of pediatrics at Children's Hospital of Pittsburgh of University of Pittsburgh Medical Center.

Comments (0)